At Bradley Physio we have over 20 years of experience treating lower limb injuries.
Pain and dysfunction in the lower limb may originate from anywhere between the spine and the little toe. Our team of highly skilled physiotherapists and sports rehabilitators are experienced in assessing and diagnosing your problem, ensuring you receive the most effective treatment possible.
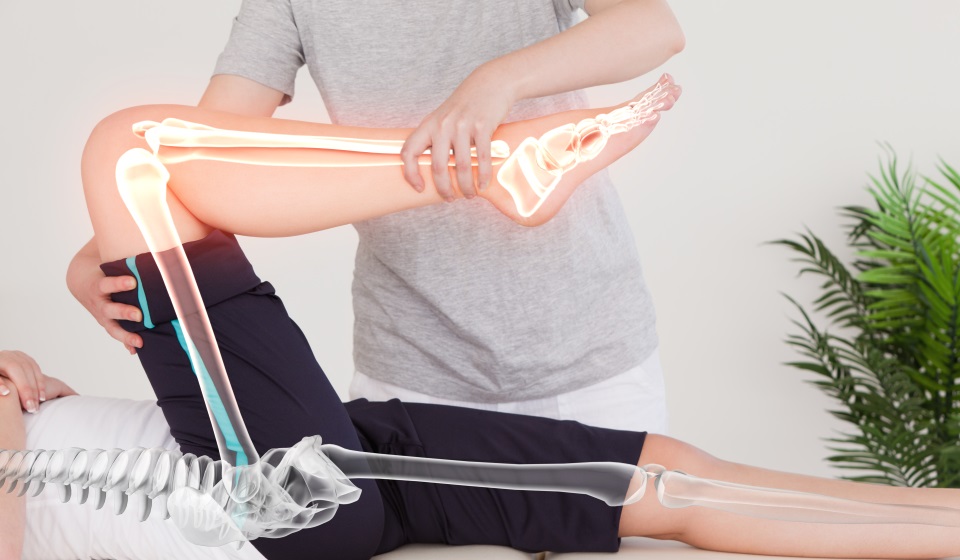
What Lower Limb Injuries do we treat?
Conditions We Treat
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays,scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Often abnormal movement patterns of the affected limb, that may have led to repetitive irritation of the bursa, need to be corrected by the careful progression of specific strengthening and stretching exercises. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. If your pain fails to settle, your therapist may discuss the option of administering a corticosteroid injection by our Specialist Physiotherapist, Patrick Bradley.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Often abnormal movement patterns of the affected limb, that may have led to repetitive irritation of the ITB, need to be corrected by the careful progression of specific strengthening and stretching exercises. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques may also be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your injury. Your recommended, bespoke treatment plan will be discussed with you. You will be advised on the use of ice if appropriate. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to an orthopaedic surgeon specialising in knee conditions the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, muscle energy techniques and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If your therapist thinks you will benefit from orthotics to correct the position of you feet to reduce the stress to the patellofemoral joint you will be advised accordingly and the necessary arrangements will be made for you.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If your therapist thinks you will benefit from orthotics to correct the position of you feet to reduce the stress on the tibia you will be advised accordingly and the necessary arrangements will be made for you.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. You will be advised on the use of ice if appropriate. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage, and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays, scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabiliator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If your pain fails to settle your clinician may discuss the option of administering a corticosteroid injection by our Specialist Physiotherapist, Patrick Bradley. If your therapist thinks you will benefit from orthotics to correct the position of you feet to reduce the stress on the tibia you will be advised accordingly and the necessary arrangements will be made for you.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If you are not making the progress we would expect and your clinician thinks you will benefit from further investigations (x-rays,scans) and/or onward referral to a doctor specialising in your condition the necessary arrangements can be made by our team on your behalf.
Following a thorough verbal and physical examination your therapist will aim to diagnose the cause of your problem. Your recommended, bespoke treatment plan will be discussed with you. Specific manual therapy techniques including deep soft tissue massage, deep transverse friction massage and stretches may be used. Other treatments may include acupuncture, electrotherapy and the use of sports tape. As you improve your physio or sports rehabilitator may recommend a programme of rehabilitation exercises in our on-site rehab gym as well as exercises and stretches to continue independently at home. We will aim to identify the cause of your injury and advise you on prevention in the future.
NOTE If your clinician thinks you will benefit from orthotics to correct the position of you feet to reduce the stress on the achilles tendon you will be advised accordingly and the necessary arrangements will be made for you.





